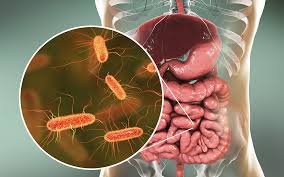
Escherichia coli – the most common cause of urinary tract infections, significant sources of gastrointestinal disease, ranging from simple diarrhea to dysentery-like conditions, neonatal meningitis, hemorrhagic colitis, and Crohn’s disease.

its a very persistent and hard to get rid of.. these natural cure is a wonder and many people said that when medications work slow or not at all these cure made their results miracle – even ,,0,, presence of Escherichia in their blood .. natural cure contains only 2 ingredients only white wine and garlic, and is easy to make home. at the end of the text instructions how to get the natural cure.
If you want to try it you just need to send us email to [email protected] for instructions
- It is the most common cause of non-nosocomial urinary tract infection (UTI).
E. coli commonly causes infections of the urinary tract in people not admitted to hospital (non-nosocomial). It is also the cause of various other infections, such as food poisoning, septicaemia, neonatal meningitis and gastroenteritis.
- E. coli causes infections by producing toxins.
In order to begin an infection, E. coli must release toxins which allow the bacterium to bind to the lining of the gut. It can then enter the body and cause symptoms of disease such as the diarrhoea associated with food poisoning.
- How severe you suffer depends on the type of E. coli you have.
E. coli exists as different types – scientists separate them as strains according to their antigens and virulence factors. The strain called O157:H7 is regarded as the most potent type of E. coli because the infection it causes can easily be fatal.
- Why is O157 infection so serious?
Scientists know that a minimum number of microbes is needed to begin an infection, called the infectious dose. Often this number is very high – many thousands of microbial cells must gain entry to the body before symptoms of infection appear. Unfortunately, E. coli O157’s infectious dose is incredibly low – just 10 E. coli cells can result in bloody diarrhoea, severe to fatal haemorrhagic colitis and the severe kidney disorder, haemolytic uremic syndrome in which the kidneys cease functioning.
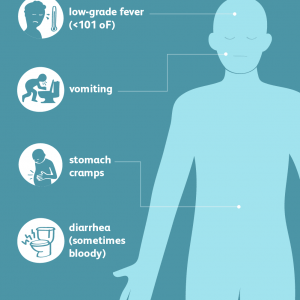 Common signs and symptoms include severe abdominal cramps, diarrhea, hemorrhagic colitis, vomiting, and sometimes fever.
Common signs and symptoms include severe abdominal cramps, diarrhea, hemorrhagic colitis, vomiting, and sometimes fever.
In rarer cases, virulent strains are also responsible for bowel necrosis (tissue death) and perforation without progressing to hemolytic-uremic syndrome, peritonitis, mastitis, septicemia, and Gram-negative pneumonia.
Very young children are more susceptible to develop severe illness, such as hemolytic uremic syndrome, however, healthy individuals of all ages are at risk to the severe consequences that may arise as a result of being infected with E. coli.
Some strains of E. coli for example O157:H7, can produce Shiga toxin (classified as a bioterrorism agent). This toxin causes premature destruction of the red blood cells, which then clog the body’s filtering system, the kidneys, causing hemolytic-uremic syndrome (HUS). In some rare cases (usually in children and the elderly) Shiga toxin producing E. Coli infection may lead to hemolytic uremic syndrome (HUS), which can cause kidney failure and even death.
Signs of hemolytic uremic syndrome, include decreased frequency of urination, lethargy, and paleness of cheeks and inside the lower eyelids. In 25% of HUS patients, complications of nervous system occur, which in turn causes strokes due to small clots of blood which lodge in capillaries in the brain. This causes the body parts controlled by this region of the brain not to work properly. In addition, this strain causes the buildup of fluid (since the kidneys do not work), leading to edema around the lungs and legs and arms. This increase in fluid buildup especially around the lungs impedes the functioning of the heart, causing an increase in blood pressure.
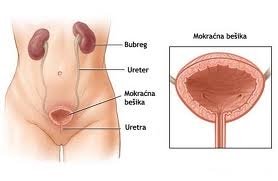
 Uropathogenic E. coli (UPEC) is one of the main causes of urinary tract infections. It is part of the normal microbiota in the gut and can be introduced in many ways. In particular for females, the direction of wiping after defecation (wiping back to front) can lead to fecal contamination of the urogenital orifices. Anal intercourse can also introduce this bacterium into the male urethra, and in switching from anal to vaginal intercourse, the male can also introduce UPEC to the female urogenital system.
Uropathogenic E. coli (UPEC) is one of the main causes of urinary tract infections. It is part of the normal microbiota in the gut and can be introduced in many ways. In particular for females, the direction of wiping after defecation (wiping back to front) can lead to fecal contamination of the urogenital orifices. Anal intercourse can also introduce this bacterium into the male urethra, and in switching from anal to vaginal intercourse, the male can also introduce UPEC to the female urogenital system.
In May 2011, one E. coli strain, O104:H4, was the subject of a bacterial outbreak that began in Germany. Certain strains of E. coli are a major cause of foodborne illness. The outbreak started when several people in Germany were infected with enterohemorrhagic E. coli (EHEC) bacteria, leading to hemolytic-uremic syndrome (HUS), a medical emergency that requires urgent treatment. The outbreak did not only concern Germany, but also 15 other countries, including regions in North America.On 30 June 2011, the German Bundesinstitut für Risikobewertung (BfR) (Federal Institute for Risk Assessment, a federal institute within the German Federal Ministry of Food, Agriculture and Consumer Protection) announced that seeds of fenugreek from Egypt were likely the cause of the EHEC outbreak.
[highlight]Incubation period
The time between ingesting the STEC bacteria and feeling sick is called the “incubation period”. The incubation period is usually 3–4 days after the exposure, but may be as short as 1 day or as long as 10 days. The symptoms often begin slowly with mild belly pain or non-bloody diarrhea that worsens over several days. HUS, if it occurs, develops an average 7 days after the first symptoms, when the diarrhea is improving.
Treatment
The mainstay of treatment is the assessment of dehydration and replacement of fluid and electrolytes. Administration of antibiotics has been shown to shorten the course of illness and duration of excretion of enterotoxigenic E. coli (ETEC) in adults in endemic areas and in traveller’s diarrhea, though the rate of resistance to commonly used antibiotics is increasing and they are generally not recommended.[78] The antibiotic used depends upon susceptibility patterns in the particular geographical region. Currently, the antibiotics of choice are fluoroquinolones or azithromycin, with an emerging role for rifaximin. Oral rifaximin, a semisynthetic rifamycin derivative, is an effective and well-tolerated antibacterial for the management of adults with non-invasive traveller’s diarrhea. Rifaximin was significantly more effective than placebo and no less effective than ciprofloxacin in reducing the duration of diarrhea. While rifaximin is effective in patients with E. coli-predominant traveller’s diarrhea, it appears ineffective in patients infected with inflammatory or invasive enteropathogens.
Prevention
 ETEC is the type of E. coli that most vaccine development efforts are focused on. Antibodies against the LT and major CFs of ETEC provide protection against LT-producing, ETEC-expressing homologous CFs. Oral inactivated vaccines consisting of toxin antigen and whole cells, i.e. the licensed recombinant cholera B subunit (rCTB)-WC cholera vaccine Dukoral, have been developed. There are currently no licensed vaccines for ETEC, though several are in various stages of development.[80] In different trials, the rCTB-WC cholera vaccine provided high (85–100%) short-term protection. An oral ETEC vaccine candidate consisting of rCTB and formalin inactivated E. coli bacteria expressing major CFs has been shown in clinical trials to be safe, immunogenic, and effective against severe diarrhoea in American travelers but not against ETEC diarrhoea in young children in Egypt. A modified ETEC vaccine consisting of recombinant E. coli strains over-expressing the major CFs and a more LT-like hybrid toxoid called LCTBA, are undergoing clinical testing.
ETEC is the type of E. coli that most vaccine development efforts are focused on. Antibodies against the LT and major CFs of ETEC provide protection against LT-producing, ETEC-expressing homologous CFs. Oral inactivated vaccines consisting of toxin antigen and whole cells, i.e. the licensed recombinant cholera B subunit (rCTB)-WC cholera vaccine Dukoral, have been developed. There are currently no licensed vaccines for ETEC, though several are in various stages of development.[80] In different trials, the rCTB-WC cholera vaccine provided high (85–100%) short-term protection. An oral ETEC vaccine candidate consisting of rCTB and formalin inactivated E. coli bacteria expressing major CFs has been shown in clinical trials to be safe, immunogenic, and effective against severe diarrhoea in American travelers but not against ETEC diarrhoea in young children in Egypt. A modified ETEC vaccine consisting of recombinant E. coli strains over-expressing the major CFs and a more LT-like hybrid toxoid called LCTBA, are undergoing clinical testing.
Other proven prevention methods for E. coli transmission include handwashing and improved sanitation and drinking water, as transmission occurs through fecal contamination of food and water supplies. Additionally, thoroughly cooking meat and avoiding consumption of raw, unpasteurized beverages, such as juices and milk are other proven methods for preventing E.coli. Lastly, avoid cross-contamination of utensils and work spaces when preparing food.
The nature is full with cure that can help fighting diseases. these cure is not substitution for medical treatment. people who use it testify that their results war 100% better.
[highlight]If you want to try it you just need to send us email to [email protected] for instructions
Medical Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this Website.
 EN.BabinLEK Cure yourself
EN.BabinLEK Cure yourself